The Revu 30th October 2017 Dr Andrew Farr talks to The Revu about his recent experience of undertaking the ITI Foundation in Implant Dentistry (FID) course and why, along with the guidance of his mentor, he is now more than ready to place his first implants. What first motivated you to attend the FID course? …
Tag Archives: Straumann
Dental Tips to Start the School Year with a Smile
With the new school year fast approaching the following back-to-school dental tips for parents are sure to help your child start the school year with a healthy smile, and keep it that way all year long. Preventing decay starts at home, so the more child-friendly your dental supplies, the more your child will love keeping up with …
Continue reading “Dental Tips to Start the School Year with a Smile”
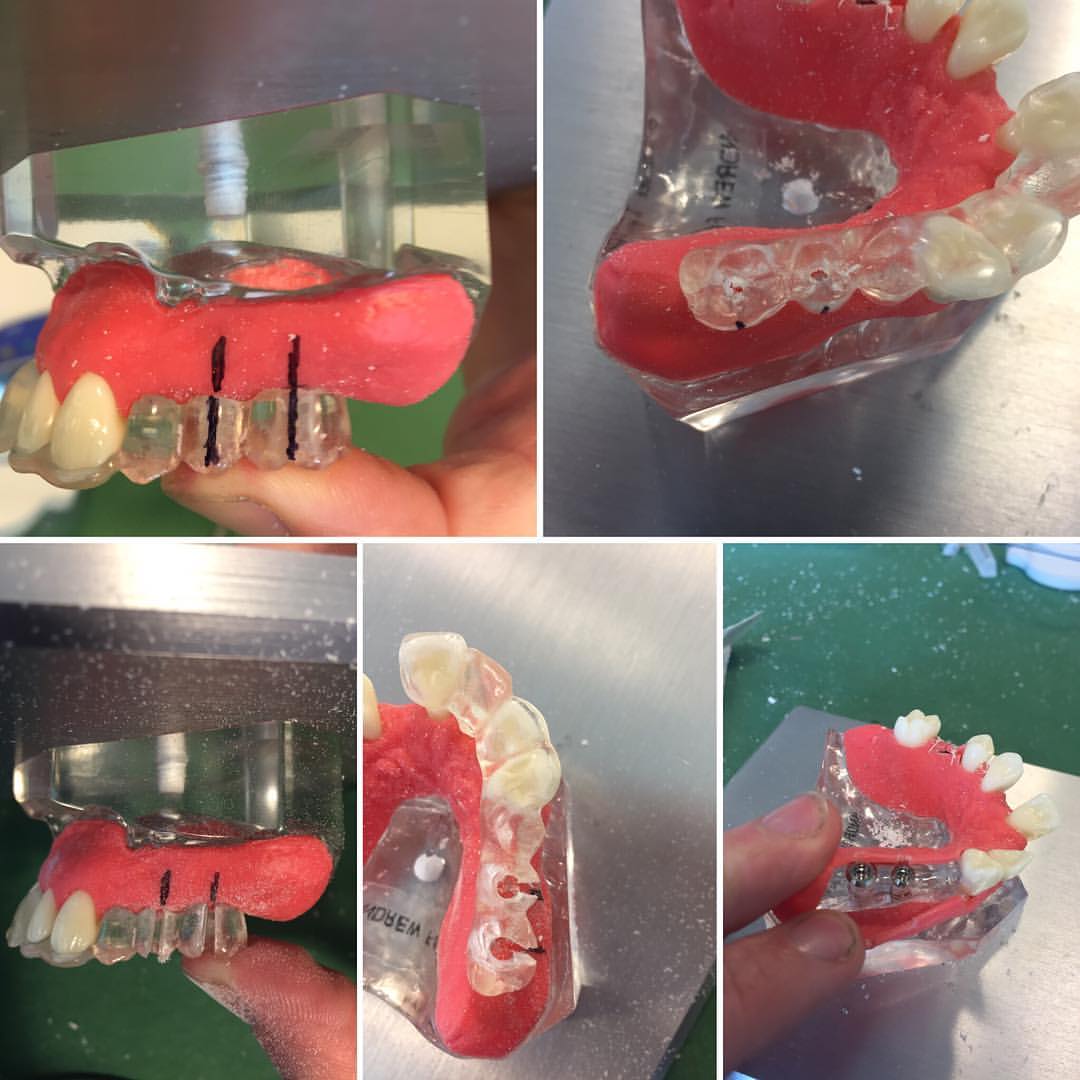
Implant Surgical Guide
A surgical guide as the name suggests serves as a guide to place implants accurately in 3 dimensions i.e. bucco-lingual, messiah-distal and apiece-coronal. Here I am showing a simple surgical guide that has been produced from an initial wax up (there are more accurate guides available). It is constructed of hard acrylic and can also …
FDI – Implant Retained Dentures
Managing the edentulous patient can be at times, very difficult. Following extraction of the dentition bone is remodelled and resorbed, muscles and ligament insertions become closer to residual ridges. This can in turn lead to an unstable and unretentive denture due to a lack of bony support. When treatment planning for the edentulous patient, it …
Foundation in Implant Dentistry Part-1
February 2017. This was the first part of the FID course held annual by the ITI (International Team for Implantology) and Straumann. The course is being held at Crawley (quite a journey from Hereford) and was easily accessible. The first module focused on Assessment and Treatment planning in Implant Dentistry. By comparing implants to other …